This Statin Study Should Have Changed Medicine—No One’s Talking About It
Statins, the most prescribed drug in the world, may be quietly disrupting key metabolic pathways. This overlooked research reveals a fix that’s simple, cheap, and almost entirely ignored.
Usually, scientific research excites me.
But this paper? It also annoyed me.
It explores how statins – the most profitable drug in history, with annual sales exceeding $20 billion – contribute to insulin resistance, increase diabetes risk, and significantly lower GLP-1 levels in humans.
Now, it's relatively well known that statins can increase insulin resistance and the risk of diabetes. But the direct, negative impact on GLP-1 levels? That was new to me.
And it caught my attention because right now, the world’s trendiest and most sought-after drugs are GLP-1 receptor agonists used for weight loss, like Ozempic and Wegovy.
So, in effect, the most profitable drug on the planet – prescribed to about 1 in 4 people >40 – may increase metabolic demand for the most popular drug class, by disrupting the same biology those drugs are trying to correct.
And here's the exciting part: there’s a simple, inexpensive solution beyond “stop the statin” or “start a GLP-1.” We’ll build to that. And I promise you won’t be disappointed.
Today, we’ll discuss:
The Overlooked Finding: The striking human data showing a ~50% drop in GLP-1 levels in statin users in a controlled trial published in a major academic journal.
The Microbiome Connection: How statins disrupt your gut to cause this negative side effect.
The Simple Solution: A pilot study in humans reveals a readily available compound that appears to reverse the damage.
Why It Matters: What this reveals about the healthcare system and how you can use this information.
Why I’m Annoyed
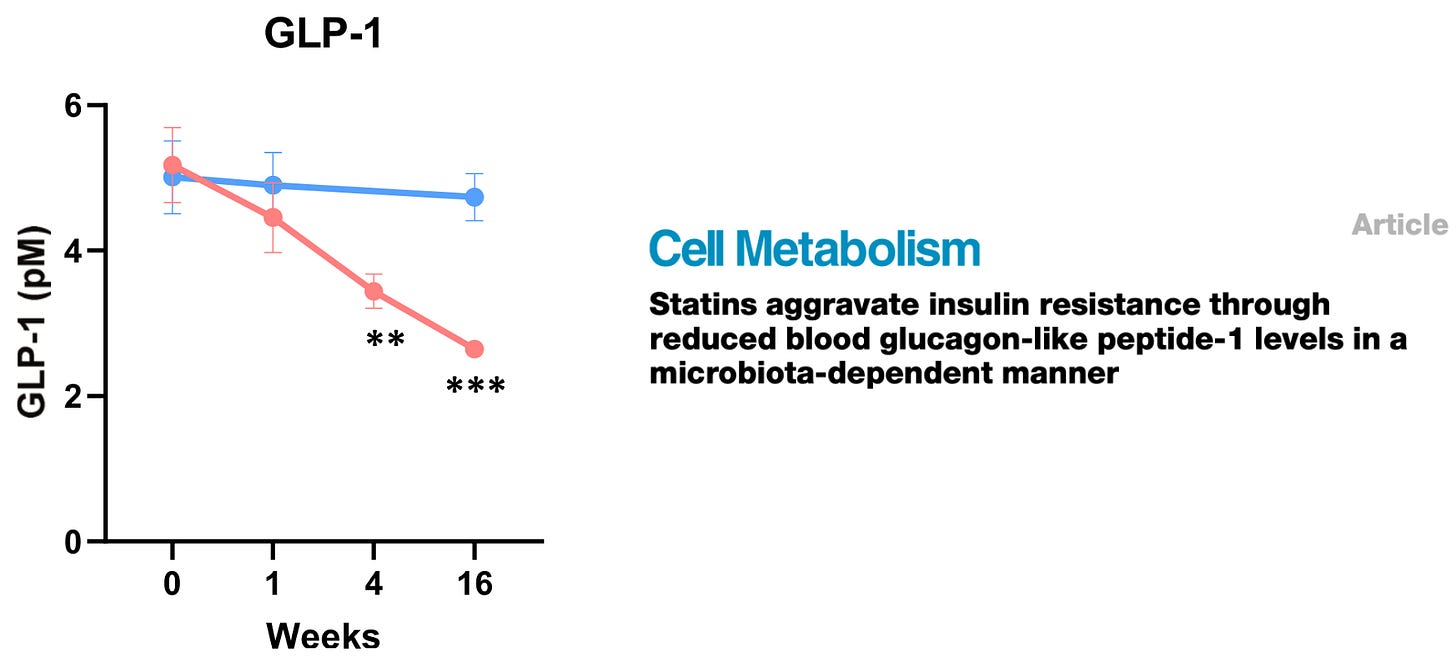
First, here’s why this paper irritated me. These findings were published over a year ago – February 6th, 2024 – in Cell Metabolism, a highly respected scientific journal. This should have been headline news, even for the general public.
At the time, I was in clinical rotations at Harvard Medical School. So, you'd think someone in my immediate environment might have mentioned it.
But no – not a word.
The day I finally found and read the paper – after reflecting on the fact that did not appear to be in the zeitgeist of academic medicine – I ran an informal poll.
I asked 12 physicians, including four cardiologists, the simple question: "What effect do statins have on GLP-1 levels?"
7 said they didn’t know. Okay, points for honesty.
The other 5 also didn’t know, but were willing to guess. 1 guessed that statins would increase GLP-1. The other 4 guessed they would lower it.
I’ll return to my impression of those responses later. But first, let’s make sure you understand more than most doctors about this overlooked finding.
What the Human Trial Showed
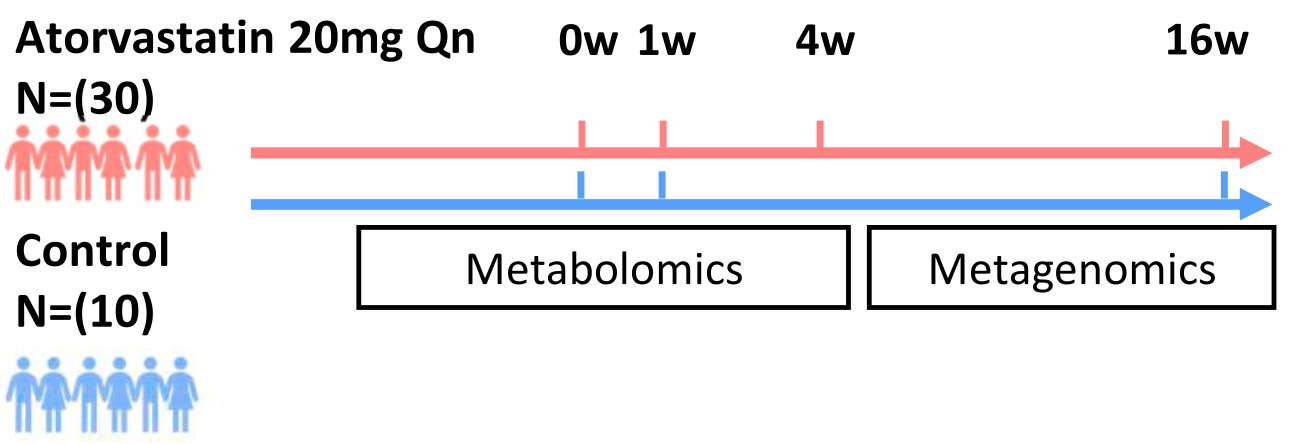
In the first experiment, researchers enrolled 30 patients who were starting atorvastatin (20 mg) and 10 control patients who weren’t taking statins. They followed both groups for 16 weeks.
The results?
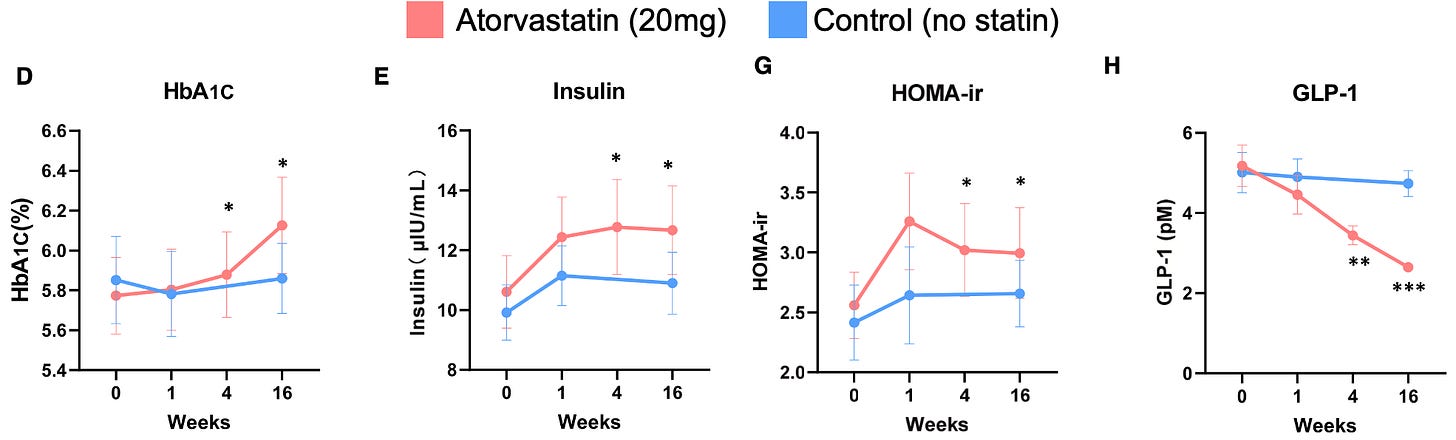
Statin use led to significant increases in HbA1c, insulin levels, and insulin resistance (measured by HOMA-IR). At the same time, it caused a sharp drop in GLP-1 – nearly 50% by the end of the four-month trial, with a continued downward trend still clearly visible.
In my opinion, just that one panel – Figure 1H from the paper (far right) – should have made headlines. Newspapers should have been shouting: “Statins cut GLP-1 levels by half! Here's what it could mean for your health.”
Here’s a thought puzzle to make the point: If you replaced “statin” with “steak,” do you think the headlines would have run? I do.
Uncovering the Mechanism: The Microbiome Connection
The researchers then dug deeper to understand how statins were exerting these negative effects. They discovered that statins altered the gut microbiome in a very specific way.
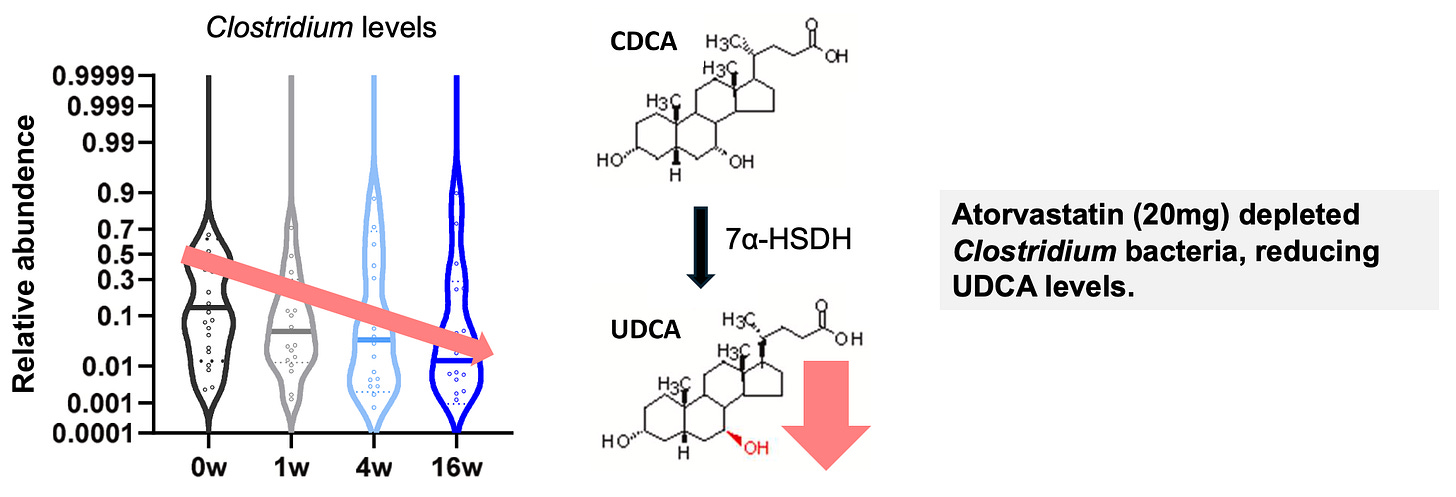
In the statin-treated patients, levels of certain secondary bile acids – compounds made by gut bacteria – had changed. Most notably, there was a marked drop in a bile acid called ursodeoxycholic acid (UDCA).
UDCA is produced when specific gut bacteria convert a precursor bile acid, CDCA, into UDCA. In this case, the main producers were Clostridium species, which express an enzyme (7α-HSDH) that performs this conversion.
Statins depleted these Clostridium bacteria, reducing the microbiome’s ability to produce UDCA. That led to downstream metabolic disruptions – including insulin resistance and reduced GLP-1 production.
Proving Causality in Mice
To confirm causality, the researchers turned to a mouse model. Just like in humans, mice given statins developed insulin resistance and showed a substantial drop in GLP-1 levels.
Furthermore, when microbiomes were transplanted from human patients who were taking statins into mice that were not, the mice developed worse insulin resistance.
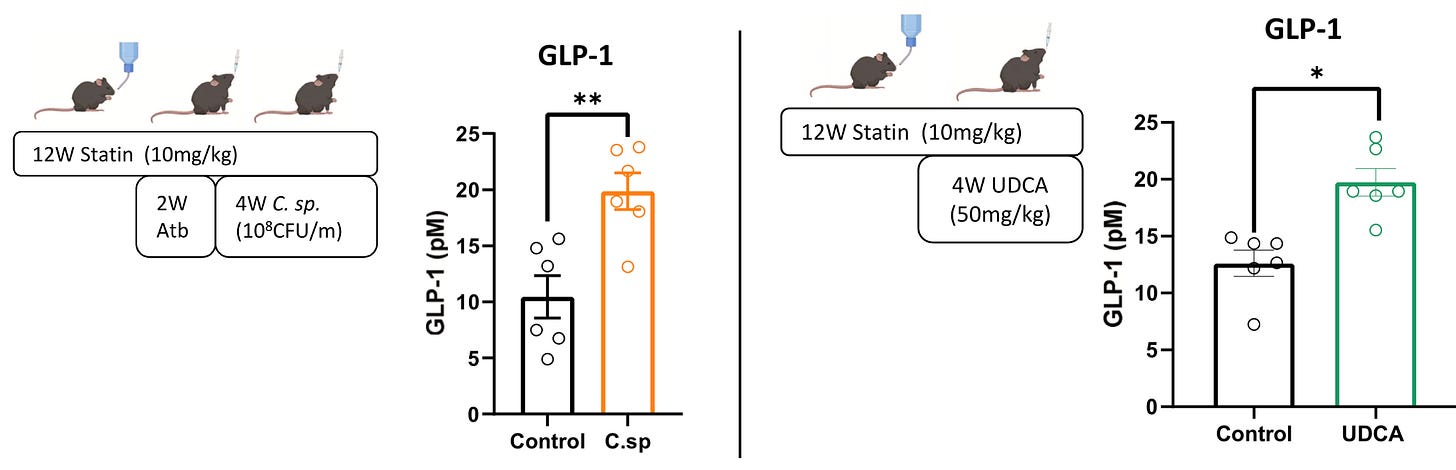
And then, when researchers either reintroduced the depleted Clostridium species or supplemented with UDCA, the metabolic damage was reversed. Glucose metabolism improved, and GLP-1 levels bounced back.
Together, these findings strongly suggest:
Statin therapy disrupts the gut microbiome by depleting key bacteria involved in bile acid metabolism.
This shift leads to reduced production of beneficial bile acids, in particular UDCA.
The consequences are insulin resistance and a sharp drop in GLP-1 levels.
These changes appear reversible with targeted intervention.
You now understand the science behind how statins disrupt the microbiome and tank GLP-1 levels—an insight that already puts you ahead of most clinicians. That’s not a slight. That’s a fact.
But the most important part is what comes next: a potential solution.
In the rest of this letter we discuss:
The Human Pilot Study: The specific, uplifting results showing how researchers reversed the metabolic harm caused by statins.
The Available Fix (It’s On Amazon? Seriously?!): How a version of this simple, inexpensive compound is already available online. (Not a Medical Recommendation. Just Information.)
A System That Can Do Better - If We Help It: My take on why this information is being ignored and what you can do to advocate for better care.